A monthly article brought to you by Senior Services Memory Support Programs
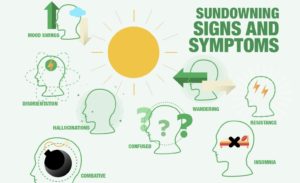
People living with dementia may have problems sleeping or experience increased confusion, anxiety, agitation, pacing, and disorientation beginning at dusk and continuing throughout the night (referred to as sundowning). Although the exact cause is unknown, these changes result from the disease’s impact on the brain.
 Many factors may contribute to sleep disturbances and sundowning. Here are some examples that may apply to your loved one.
Many factors may contribute to sleep disturbances and sundowning. Here are some examples that may apply to your loved one.
Mental and physical exhaustion from a full day trying to keep up with an unfamiliar or confusing environment.
- An upset in the “internal body clock,” causing a biological mix-up between day and night.
- Reduced lighting can increase shadows and may cause the person living with the disease to misinterpret what they see and, subsequently, become more agitated.
- Nonverbal behaviors of others, especially if stress or frustration is present, may inadvertently contribute to the stress level of the person living with dementia.
- Disorientation due to the inability to separate dreams from reality when sleeping.
- Less need for sleep, which is common among older adults.
If your loved one is experiencing sleep disturbances and sundowning, what can you do to best support them through this challenging behavior?
- Get plenty of rest so you are less likely to exhibit unintended nonverbal behavior.
- Schedule activities such as doctor appointments, trips, and bathing in the morning or early afternoon hours when the person living with dementia is more alert.
- As much as possible, encourage a routine of waking up, meals, and going to bed.
- When possible and appropriate, include walks or time outside in the sunlight.
- Make notes about what happens before sundowning events and try to identify triggers.
- Reduce stimulation during the evening hours (i.e., TV, doing chores, loud music, etc.). These distractions may add to the person’s confusion.
- Offer a larger meal at lunch and keep the evening meal lighter.
- Keep the home well lit in the evening. Adequate lighting may reduce the person’s confusion.
- Do not physically restrain the person; it can make agitation worse.
- Try to identify activities that are soothing to the person, such as listening to calming music, looking at photographs, or watching a favorite movie.
- Take a walk with the person to help reduce his or her restlessness.
- Talk to the physician about the best times of day for taking medication.
- If the person has trouble sleeping at night, it can be helpful to limit daytime naps.
- Reduce or avoid alcohol, caffeine, and nicotine, which can all affect the ability to sleep.
If the person is awake and upset, what should you do?
- Calmly approach him or her.
- Find out if there is something he or she needs (ex: a drink, to use the bathroom)
- Gently remind him or her of the time.
- Avoid arguing.
- Offer reassurance that everything is all right.
- Do not use physical restraint. Allow the person to pace back and forth, as needed, with supervision.
If the person gets up in the middle of the night, gets dressed, and tries to go outside, what should you do?
- Put a clock by the bed and set the alarm. You might say, “You can get out of bed when the clock beeps.”
- You can install a bedroom door or outdoor alarm to wake you when he or she tries to go outside.
- Assist your loved one back into bed. Soothe the person until he or she falls asleep again or relaxes and stays in bed. Play a piece of favorite music or read aloud softly.
When behavioral interventions and environmental changes do not work, discuss the situation with your doctor.
Discuss sleep disturbances with a doctor to help identify causes and possible solutions. Physical ailments, such as urinary tract infections or incontinence problems, restless leg syndrome, or sleep apnea, can cause or worsen sleep problems. For sleep issues due primarily to dementia, most experts encourage the use of non-drug measures rather than medication.
In some cases when non-drug approaches fail, medication may be prescribed for agitation during the late afternoon and evening hours. Work with the doctor to learn the risks and benefits of medication before making a decision.
Some research suggests that a low dose of melatonin — a naturally occurring hormone that induces sleepiness — alone or in combination with exposure to bright light during the day may help ease sundowning.
When you start to notice memory changes, seeking early detection is key. Senior Services offers an array of memory support programs including confidential memory screenings to obtain a cognitive baseline, early memory loss programs, consultations, and educational classes along with support from Seasons Adult Day Health Services. If you or someone you know is experiencing increasing changes with their memory and could benefit from additional services, please contact Amy Sheridan, Family Support and Activity Manager at 989-633-3764.
Check out our section, Our Mind Matters, next month as we discuss wandering and rummaging.

